Filippo Pieralli1,2 *, Simona Barbaglia3 *, Ovidio Brignoli4, Lorenzo Cottini5,6, Francesca Moccia7
1Internal Medicine and Intermediate Care Unit – General and University Hospital Careggi, Firenze
2Italian Scientific Society of Internal Medicine FADOI
(Federazione delle Associazioni dei Dirigenti Ospedalieri Internisti)
3National Association of Patients “Respiriamo Insieme” (“Let’s breath together”) Non Profit Organzation, Padova
4Italian Society of General Medicine and Primary Care
(Società Italiana di Medicina Generale e delle Cure Primarie – SIMG)
5Association of Industrial Pharmacists (Associazione Farmaceutici Industria – AFI)
6High Research srl, Milano
7Cittadinanzattiva Non-Profit Organization, Roma
*The two Authors contributed equally to the drafting of the manuscript
Tendenze nuove, Numero Speciale 4 2021; 201-216: DOI: 10.32032/TENDENZENUOVENS04202114.PDF

Digital health (DH) comprises the use of information and communication technology (ICT) to treat and educate citizens, carry out research, train healthcare providers, track diseases and monitor public health. DH stands at the crossroads of digital technologies, medicine, healthcare, lifestyle and society, the aim being to ensure more efficient, personalized and precise delivery of treatment.
DH is constantly evolving and growing, the number of medical apps having doubled from 2015 to 2018. The World Health Organization (WHO) decided in 2018 that it was time to set up a classification of DH. The field as a whole was thus broken down into four main areas of interest, based on the targeted primary user and the aim of the intervention(1). The four groups, closely related and interconnected, are as follows:
Interventions for clients: Clients are members of the public who are potential or current users of health services, including health promotion activities. Caregivers of clients receiving health services are also included in this group.
Interventions for healthcare providers: Healthcare providers are members of the health alliance who directly or indirectly deliver health services.
Interventions for health system or resource managers: Health system and resource managers are involved in the administration and oversight of public health systems. Interventions within this category reflect managerial functions related to supply chain management, health funding and human resource management.
Interventions for data services: This consists of crosscutting functionality to support a wide range of activities related to data collection, management, use and exchange (big data).
From this classification of DH, it is clear that Scientific Societies and Associations of Patients/Family Members can be directly interested and involved in the use, promotion and development of DH.
What Scientific Societies and Associations of Patients & Family Members think and are doing
Analysis of data collected through a web-based search has enabled us to establish that Scientific Societies are generally very interested in DH, even if few of them have issued position statements or guidelines regarding this field.
A 2015 WHO survey of mobile health (mHealth) apps found that about 30% of them deal with diagnosis, treatment and support for mental disorders. Some of these tools have been included in treatment guidelines – in the United Kingdom, for example, two digitalized interventions are recommended for treatment of mental disorders (Beating the Blues® for depression; FearFighter, for panic and phobia). The World Psychiatric Association (WPA) was among the first Scientific Societies to address the question(2)and issue a position statement on mental health in the digital age, which it calls e-Mental Health (e-MH)(3). This definition of e-MH applies generally to the overall field of digital technology used in supporting, delivering and improving the mental health and well-being of individuals with psychiatric disorders. Outlining the rationale and potential for using digital systems to treat mental conditions, the document looks at clinical, research, educational and administrative perspectives. The models need to be integrated with traditional practice, to better identify at-risk subjects, awareness and management of mental illness, prevention and early identification of relapses.
Of note, in the field of psychiatric disorders, digital technology can contribute to diagnosis and monitoring, and enhance perception and awareness of disease. A proactive approach is characteristic of e-MH, the aim being to transform the patient’s role and experience while integrating different treatments. In addition, as for all DH, there is also the advantage of reducing time and space barriers, particularly in more difficult community settings.
The extent to which technology is used for e-MH, as indeed for DH in general, is evolving very rapidly even if in a spotty and relatively unregulated manner. A recently published meta-analysis of adherence to clinical guidelines examines apps used on iOS and Android platforms, for suicide prevention and suicide risk assessment in patients with depression(4). Of 69 apps analysed, accounting for a total of 2 million downloads, the analysis shows that 20 (29%) were for management of depression, 3 (4%) for management of depression and suicide prevention, and 46 (67%) for suicide prevention. Only 5 of the 69 apps (7%) offered strategies recommended as the result of evidence-based investigation. In addition, many of the apps in the analysis provided psychiatric emergency contact numbers that were non-existent or wrong. These findings show that manufacturers and app stores have failed to guarantee the necessary quality and safety controls, a trend that should be carefully addressed and that strongly calls for appropriate corrective measuresto ensure appropriateness and to avoid commercial distortions.
One of the Scientific Societies that has been most active in addressing the implications of DH is the European Society of Cardiology (ESC), as highlighted by its March 2019 “ESC e-Cardiology Working Group Position Paper: Overcoming challenges in digital health implementation in cardiovascular medicine”(5). This position paper was developed in collaboration with other Scientific Societies and Associations in the cardiovascular field (European Association of Preventive Cardiology, European Heart Rhythm Association, Heart Failure Association, European Association of Cardiovascular Imaging, Acute Cardiovascular Care Association, European Association of Percutaneous Cardiovascular Interventions, Association of Cardiovascular Nursing and Allied Professions, Council on Hypertension). Essentially, the paper underlines how DH can play an extremely important role in enhancing the quality and accessibility of healthcare for patients with, or at risk of cardiovascular disease.
The ESC’s position paper is in line with its mission and strategic plan, one aim of which is to cover all facets of support for the electronic cardiovascular health agenda in Europe. To this end, the paper is intended as a source of guidance for cardiologists and other stakeholders in the cardiovascular and DH fields. Looking at currently available applications for cardiovascular disease, the document identifies a number of possible challenges to the implementation of DH. One such barrier is the perception among healthcare professionals that heavy time investments are needed to review incoming data and provide patients with feedback: a case in point is the use of telemonitoring programmes for heart failure, which are set up without reducing or adapting the frequency of conventional hospital-based appointments. Further challenges to DH’s implementation and development are the paucity of adequate infrastructure and networks, the lack of clearly regulated and standardized procedures, and the need for greater DH expertise and education of healthcare providers.
The American College of Cardiology has also set out a number of principles for support to DH initiatives(6), the main points of which can be summarized as follows:
• enable patient engagement and shared decision-making in care delivery, by providing clinicians and patients with improved access to personalizedhealth information;
• conduct research into appropriate use of DH and its integration into cardiovascular care, to ensure patient safety, care quality and positive health outcomes;
• improve patient experience, care quality, patient safety and outcomes without hampering the clinical workflow;
• foster the development, adoption and evolution of practices that optimize data security, privacy, use and sharing, as well as device security and safety;
• adopt and utilize standardized approaches for seamless data transmission, integration, aggregation and analysis (big data analysis).
In Italy, the Internal Medicine Society FADOI (Federazione delle Associazioni dei Dirigenti Ospedalieri Internisti) has always taken an active interest in DH questions, inter aliadeveloping an app with diagnostic and therapeutic algorithms for some of the main conditions within the internist’s purview (FADOI Guides), and even running an advanced DH course in September 2019 (Scuola di Alta Formazione sul ragionamento clinico in era digitale, held in Bologna).
In General Medicine, Italy’s Federazione Italiana dei Medici di Medicina Generale(FIMMG) dedicated time at its October 2020 National Congress to presentation of a DH survey among the physicians it represents. Respondents’ opinions were sought on various aspects of DH, with a view to subsequent drafting of a position paper. The main findings of the survey can be summarized as follows:
a. digital solutions (apps, use of digital diagnosis and treatment systems) should be “prescribed” and overseen by the doctor, like any other form of diagnosis and treatment;
b. information and data generated by “DH and digital medicine solutions” should be pooled and integrated with healthcare data in General Practitioners’s (GP) databases;
c. “DH and digital medicine solutions” are considered by physicians as an opportunity to improve accessibility to health services (with even broader scope at community level, where they are available at the patient’s home and GP’s office), extending doctor-patient contact and communication;
d. The use of these resources underpins the need for clear, consistent processes, procedures and regulatory frameworks, to guarantee patient safety and ensure that healthcare providers have a full understanding of related medical liability issues. This is also the reasoning behind the recommendation that the solutions proposed should be accredited and subject to adequate and sound certification processes.
Among Patients’ Associations, those in the respiratory area were in favour of developing digital medicine technology, confidently expecting significant benefits for the patient’s quality of life, particularly in terms of their fundamental right to be treated as far as possible at home.
More generally, a survey of third sector organizations in Italy showed a steady increase since 2016 in the attention and interest prompted by DH opportunities, with scope for development of original and concrete solutions to improve the daily life and health of people with chronic, disabling disease. Projects promoted and supported by Patients’ Associations in the last three years have started to be conceived more and more as product-service solutions with a tangible potential impact on the patient’s lifestyle and daily life. There is an increasing drive to involve patients and their families in the design and development processes underpinning these new technologies. One of the main aims of Patients’ Associations is increasingly to promote, stimulate and support projects and initiatives developed by patients and caregivers, in collaboration with developers and manufacturers, digital technology laboratories and start-ups, pooling the various stakeholders’ specific know-how and leveraging the passion they share.
We therefore set out to review experience acquired in Italy, from 2017 to date, with innovative DH solutions involving Patients’ Associations and the patients themselves. This enabled us to identify a total of 150 projects, in each case looking at details of the digital product and/or service concerned. Of the 150 solutions thus identified, about 47% (71/150) include a service component (application, platform); while about 20% (31/150), as pure service solutions, are wholly digital in nature.
Three examples of significant experiences in this setting are:
• DEEBEE.IT YAGI: a tool for monitoring children’s blood sugar levels, developed by the diabetes Association of the same name. This is an open computer system for remote, real-time online visualization of values identified by a blood sugar sensor, allowing children with diabetes to attend school safely. Remote monitoring allows the doctor or a family member to track blood sugar levels even on a personal computer, smartphone or smartwatch;
• TASKABILE: a free app that runs on a smartphone or tablet, for persons with intellectual and interpersonal disabilities, developed by the Veneto region chapter of ANGSA (Associazione Nazionale Genitori Soggetti Autistici). The aim is to stimulate and facilitate learning of logical sequences, helping to acquire certain skills for everyday life and social interaction. This goes hand in hand with promoting self-sufficiency, making it possible to communicate and execute choices by means of personalized/personalizable categories and images;
• SAFE@HOME: self-sufficient living becomes reality. A prototype house that, thanks to sensors and a cloud platform, makes reports and alerts available to caregivers, healthcare providers and technical/maintenance staff. Guarantees continuity of care and assistance for persons with cognitive deterioration.
Italian digital therapeutics survey (Terapie Digitali per l’Italia – #DTxITA)
We ran the survey in July 2020, together with Fondazione SmithKline as promoter of the Terapie Digitali per l’Italia – #DTxITAproject and the FADOIScientific Society’s Clinical Research Department. The aim of the survey, based on a questionnaire for Scientific Societies/Associations and Patients’ Associations, was to investigate patients’ awareness and experience (if any) of DH activities, together with their opinion of prospects for digital therapeutics (DTx), both generally and with specific reference to Italy.
The questionnaire was completed and returned by 24 Scientific Societies/Associations and 11 Patients’ Associations (see list in Appendix), accounting for a response rate of about 40%. Responses received are summarized below, in Tables 1 and 2.
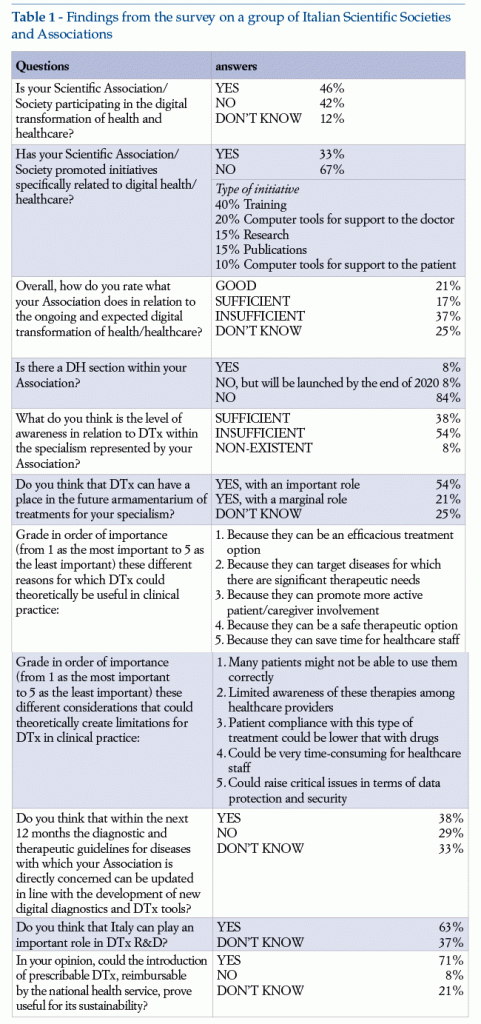
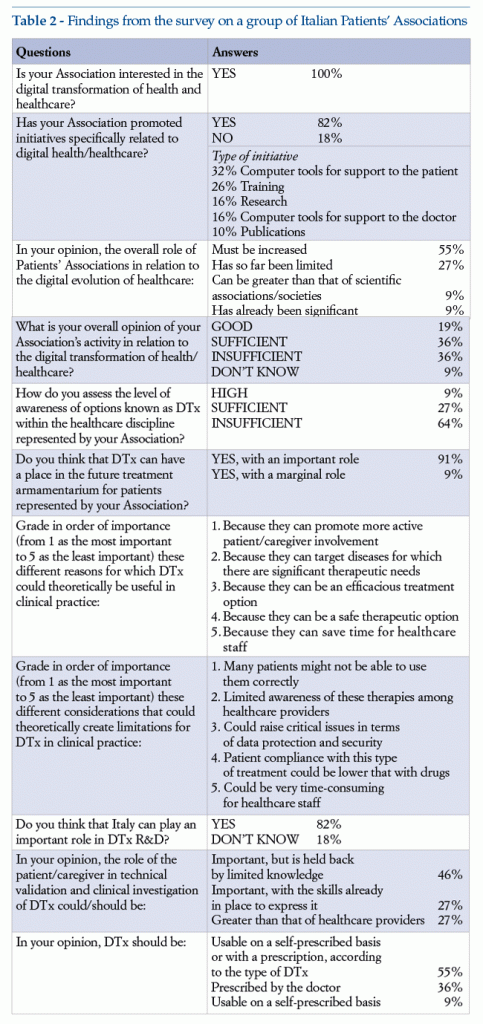
Starting from the basic premise that the tendency in this type of survey is usually for respondents to be those with greater awareness and interest in relation to the topic, thus creating a selection bias, Scientific Associations – and, even more so, Patients’ Associations – generally show significant interest in DH as a whole and in DTx spcifically. Even if some Associations state that they have already developed specific initiatives in DH, those in the survey recognize overall that awareness and commitment in relation to all these topics has so far been limited. Regarding DTx in particular, Scientific Societies consider that their potential efficacy makes them an interesting option for clinical practice, above all for conditions with major treatment unmet needs and consequent room for improvement; Patients’ Associations, in addition to these aspects, underline how important it is to have treatments available that presuppose active involvement of patients and caregivers. Both for healthcare providers’ and for Patients’ Associations, the main potential limitations of DTx are the inability of many patients to use them correctly and the limited specific know-how among healthcare providers. In all cases, Patients’ Associations consider that the patient must have a very important role in initial investigation of DTx. Most Scientific and Patients’ Associations are confident that Italy can play an important role in the development of DTx, and that dissemination of this technology can contribute positively to the sustainability of the national health service.
Conclusions
Summing up, the medical and scientific community shows great interest and curiosity in relation to the development, promotion and integration of DH. It is seen as an opportunity not only to treat and educate citizens but also to carry out research, with obvious advantages in terms of acquiring and managing large masses of data, training healthcare providers, tracking diseases, and facilitating patients’/citizens’ involvement so as to enhance awareness, promotion of health and management of diseases. With DH becoming an increasingly important part of healthcare, it has enormous potential for development in all its forms and applications. Its promotion could bring extremely important benefits to complex health systems, with ageing populations that suffer from chronic diseases and need frequent reassessments and adjustments of treatment. The spontaneous and disorganized flourishing of DH underlines the need for a well organized playing field with clear regulatory requirements, good coordination and structured contributions, within a health system that fulfils the necessary criteria in terms of know-how, orderly and well-planned integration of hardware/software, etc. In a recent Technology Review Insights survey, run by the Massachusetts Institute of Technology in collaboration with GE Healthcare, more than 900 UK and US healthcare providers saw the application of DH as an advantageous time-saving resource for medical staff, meaning a less crowded schedule for talking to patients and carrying out other procedures. Most respondents also reported that use of artificial intelligence improves the accuracy of predictions and leaves less margin of error in treatment of diseases. These indications are certainly encouraging, but, as already underlined by authoritative sources such as the US National Academy of Medicine, high quality standards must be guaranteed for data, and there must be specific legislative regulation of the DH sector as a whole(7). In this way, DH should bring a prospect of real benefits not only in strictly clinical terms, but also for health systems as a whole. This makes it necessary to guard against the risk of its piecemeal, unplanned and insufficiently resourced introduction into clinical practice, with a counterproductive effect on the workflow (e.g., lack of a dedicated time slot for analysing remotely transmitted/processed data, thus making further demands on an already full daily workload). Greater control and a regulatory certification process are thus needed, guaranteeing quality and security of access to open platforms for downloads of health-related software that could affect people’s health. Actually, without appropriate controls from third parties and regulatory oversight, there is a substantial risk that many new tools will find their way into use mainly for commercial purposes rather than for sound and appropriate evidence-based reasons, with potentially harmful fallout for all the actors involved in the healthcare system chain. DH is an extraordinary opportunity that needs to be overseen and regulated, just as a river is a precious source of water but will often need close monitoring to avoid dangerous flooding when swollen by heavy rainfall.
What is known
• Digital health is a constantly evolving and growing phenomenon
• One of the sectors where digital health has developed most is treatment of mental disorders. However, the rapid evolution of digital health has been accompanied by piecemeal, relatively unregulated availability of technology for medical use, with evidence-based strategies more the exception than the rule
• Given the scale and the sensitive nature of this phenomenon, Scientific Societies and Patients’/Family Members’ Associations should be directly involved in the use, promotion and development of technology in the digital health sector
• Even internationally, initiatives by Scientific and Patients’ Associations to promote education and research, as well as more extensive awareness raising and analysis, are still rather limited, particularly in the specific sector of digital therapeutics.
What is uncertain
• Promotion of digital health can bring very important benefits to increasingly complex health systems, but it is imperative that the environment should be conducive to this in terms of skills, orderly and well-planned integration of hardware/software, etc
• Outstanding issues include the perception that digital health, without adequate investment and infrastructure, can raise demands on healthcare providers’ time because of the increasing information load to manage, with foreseeable implications for the successful use of digital technology in the health field
• Further issues are the availability of adequate, efficient infrastructure and networks, the need for a regulatory framework and standardized procedures, and the importance of promoting digital health awareness and education among healthcare providers.
What we recommend
• To protect all stakeholders, from the patient to the doctor to the healthcare organization, there must be a guarantee that digital technologies applicable to healthcare are adequately regulated and supported by specific legislation
• Associations of Patients/Family Members and Scientific Associations should take on an independent, more active role in fully developing the opportunities afforded by digital technologies
• With specific reference to digital therapeutics, Patients’/Family Members’ Associations and Scientific Societies can play an important part in investigating devices, as well as for the necessary awareness raising and training – both for users (patients and caregivers) and for potential prescribers (healthcare providers)
• Italy can play a significant part in the rapidly evolving field of digital technology for health, and the active role we recommend for Associations should be developed in a timely and coordinated manner.
Appendix
List of Patients’ Associations participating in the “Terapie Digitali per l’Italia – #DTxITA” survey
(The following acronyms are used where applicable: NPO = Non-Profit Organization; ‘APS’ = Italian acronym for ‘Associazione di Promozione Sociale’ – i.e., legally recognized Association for Social Support)
• AAI – Associazione Apnoici Italiani Onlus – APS
(Italian Sleep Apnoea Association – NPO / APS)
• AAL – Associazione Allergici al Lattice
(Latex Allergy Association)
• ACTO – Alleanza contro il Tumore Ovarico
(Alliance against Ovarian Tumours)
• ADPMI – Associazione Diabetici della Provincia di Milano Onlus
(Association of Diabetics of the Province of Milan – NPO)
• AIP O.d.V. – Associazione Immunodeficienze Primitive
(Association for Primary Immunodeficiencies)
• AMIP – Associazione Malati di Ipertensione Polmonare Onlus
(Association of Pulmonary Hypertension Patients – NPO)
•ANMAR – Associazione Nazionale Malati Reumatici Onlus
(National Association of Patients with Rheumatic Diseases – NPO)
• APMARR – Associazione Nazionale Persone con Malattie Reumatologiche e Rare – APS
(National Association of Persons with Rheumatological and Rare Diseases – APS)
• Associazione Italiana Pazienti BPCO Onlus
(Italian Association of COPD Patients – NPO)
• FIE – Federazione Italiana Epilessie
(Italian Epilepsy Federation)
• GILS – Gruppo Italiano Lotta alla Sclerodermia
(Italian Group against Systemic Sclerosis)
List of Scientific Societies / Associations participating in the “Terapie Digitali per l’Italia – #DTxITA” survey
(The following acronym is used where applicable: NPO = Non-Profit Organization)
• ACOI – Associazione Chirurghi Ospedalieri Italiani
(Association of Italian Hospital Surgeons)
• AIOM – Associazione Italiana di Oncologia Medica
(Italian Association of Medical Oncology)
• AME – Associazione Medici Endocrinologi
(Association of Endocrinological Specialists)
• CIPOMO – Collegio Italiano dei Primari Oncologi Medici
(Italian College of Directors ofMedical Oncology)
• FADOI – Federazione delle Associazioni dei Dirigenti Ospedalieri Internisti
(Federation of Associations of Internal Medicine Clinicians)
• FICOG – Federation Italian Cooperative Oncology Groups
• FIV – Fondazione Italiana Vascolare Onlus
(Italian Vascular Foundation – NPO)
• Fondazione NIBIT Onlus – Network Italiano per la Bioterapia dei Tumori
(NIBIT Foundation – NPO/Italian Network for Tumour Biotherapy)
• Fondazione Policlinico di Monza
(Foundation of the Monza Polyclinic)
• GISCAD – Gruppo Italiano per lo Studio dei Carcinomi dell’Apparato Digerente
(Italian Group for Study of Digestive Tract Carcinomas)
• Hunimed – Istituto Clinico Humanitas– Humanitas University
(Humanitas Clinical Institute – Humanitas University)
• IGG – Gruppo Italiano Tumori Germinali
(Italian Germinal Cell Tumour Group)
• IMI – Intergruppo Melanoma Italiano
(Italian Melanoma Joint Group)
• MaNGOGroup – Mario Negri Gynecologic Oncology Group
• Meet-Uro – Italian Network for Research in Urologic Oncology
• MITO – Multicenter Italian Trials in Ovarian Cancer
• SIC – Società Italiana di Chirurgia
(Italian Society of Surgery)
• SIDV – Società Italiana Diagnostica Vascolare
(Italian Society of Vascular Diagnostics)
• SIFO – Società Italiana di Farmacia Ospedaliera e dei Servizi Farmaceutici
(Italian Hospital Pharmacy / Pharmaceutical Services Society)
• SIGG – Società Italiana di Gerontologia e Geriatria
(Italian Society of Gerontology and Geriatrics)
• SIGOT – Società Italiana Geriatria Ospedale e Territorio
(Italian Society of Hospital and Community Geriatrics)
• SIMV – Società Italiana di Medicina Vascolare
(Italian Vascular Medicine Society)
• SIP – Società Italiana di Pediatria
(Italian Paediatrics Society)
• SIR – Società Italiana di Reumatologia
(Italian Society of Rheumatology)
Acknowledgments
The authors would like to thank Elisa Zagarrì and Giuseppe Oteri (Dipartimento per la Ricerca Clinica “Centro Studi FADOI”, Milano) for their greatly valued cooperation with the Terapie Digitali per l’Italia – #DTxITAsurvey of Scientific Societies/Associations and Patients’/Family Members’ Associations.
Bibliography
1.World Health Organization. Classification of digital health interventions v1.0: a shared language to describe the uses of digital technology for health. 2018.
2.Maron E, Baldwin DS, Balõtšev R, et al. Manifesto for an international digital mental health network. Dig Psyc2019; 1: 14-24.
3.World Psychiatric Association. WPA Position Statement on e-Mental Health. October 2017 https://3ba346de-fde6-473f-b1da-36498661f9c. filesusr.com/ugd/e172f3_6c100e940fbc4c6e91a79c9cdd98193d.pdf
4.Martinengo L, Van Galen L, Lum E, et al. Suicide prevention and depression apps’ suicide risk assessment and management: a systematic assessment of adherence to clinical guidelines. BMC Med 2019; 17: 231.
5.Frederix I, Caiani EG, Dendale P, et al. ESC e-Cardiology Working Group Position Paper: Overcoming challenges in digital health implementation in cardiovascular medicine. Eur J Prev Cardiol 2019; 26: 1166-77.
6.Bhavnani SP, Parakh K, Atreja A, et al. 2017 Roadmap for Innovation – ACC Health Policy Statement on healthcare transformation in the era of digital health, big data, and precision health: a report of the American College of Cardiology Task Force on Health Policy Statements and Systems of Care. J Am Coll Cardiol 2017; 70: 2696-2718.
7.Corciella R. Con l’intelligenza artificiale i medici possono già dedicare più tempo a malati e cure. www.corriere.it, 28 February 2020.
List of Authors of the book “Digital therapeutics: an opportunity for Italy, but not only” and of Members of the Team for the Project “Digital Therapeutics for Italy – #DTxITA”
•Italia Agresta – European Patients’ Academy/EUPATI Non-Profit Organization and Italian national Association of People with Rheumatological and Rare Diseases (Associazione Nazionale Persone con Malattie Reumatologiche e Rare – APMARR)
•Roberto Ascione – Healthware Group, Salerno
•Simona Barbaglia – National Association of Patients “Respiriamo Insieme” (“Let’s breath together”) Non Profit Organization, Padova
•Paolo Barbanti – Pharma & Biotech Advisors srl, Milano
•Marcella Bellani –Department of Neurosciences, Biomedicine and Movement, University of Verona
•Elio Borgonovi – CERGAS, SDA Bocconi School of Management, Milano and Smith Kline Foundation, Verona
•Paolo Brambilla – Department of Medico-Surgical Physiopathology and Transplants, University of Milan
•Ovidio Brignoli – Italian Society of General Medicine and Primary Care (Società Italiana di Medicina Generale e delle Cure Primarie – SIMG)
•Alessio Brunello – GlobalData Plc, London, United Kingdom
•Federico Cabitza – Department of Informatics, Systems and Communication, University of Milano-Bicocca
•Enrico Caiani – Politecnico di Milano, Electronics, Information and Biomedical Engineering Department
•Silvia Calabria – Fondazione ReS (Ricerca e Salute) – Research and Health Foundation, Casalecchio di Reno (Bologna)
•Emiliano Casalicchio – Computer Science Department, Sapienza University, Roma
•Oriana Ciani – CERGAS, SDA Bocconi School of Management, Milano
•Lorenzo Cottini – Association of Industrial Pharmacists (Associazione Farmaceutici Industria – AFI), Milano and High Research srl, Milano
•Salvatore Crisafulli – Department of Biomedical Sciences, Dentistry and Morphological and Functional Imaging, University of Messina and Italian Society of Pharmacology (Società Italiana di Farmacologia – SIF)
•Lucio Da Ros – Smith Kline Foundation, Verona
•Antonio Ferrari – IQVIA Ltd, Durham, NC, United States
•Sebastiano Filetti – School of Health, UnitelmaSapienza, Roma
•Sabrina Grigolo – European Patients’ Academy / EUPATI Non-Profit Organization
•Gualberto Gussoni – Department for Clinical Research “Centro Studi” FADOI (Italian Scientific Society of Internal Medicine), Milano
•Emanuele Lettieri – Department of Management Engineering, University “Politecnico” of Milano
•Felice Lopane – Life Sciences, Assolombarda, Milano
•Alberto Malva – Italian Society of General Medicine and Prmary Care (Società Italiana di Medicina Generale e delle Cure Primarie – SIMG) and Smith Kline Foundation, Verona
•Luigi V. Mancini – Computer Science Department, Sapienza University, Roma
•Chiara Mannelli – Candiolo Cancer Institute, FPO-IRCCS, Candiolo (TO)
•Nello Martini – Fondazione ReS (Ricerca e Salute) – Research and Health Foundation, Casalecchio di Reno (Bologna)
•Stefano Mazzariol – European Patients’ Academy/EUPATI Non-Profit Organization
•Alessandro Mei – Computer Science Department, Sapienza University, Roma
•Francesca Moccia – Cittadinanzattiva Non-Profit Organization, Roma
•Giulio Pagnotta – Computer Science Department, Sapienza University, Roma
•Luca Pani – Department of Biomedical & Metabolical Sciences and Neurosciences, University of Modena and Reggio Emilia; Department of Psychiatry and Behavioral Sciences, Leonard M. Miller School of Medicine – University of Miami; VeraSci, Durham, USA andItalian Society of Pharmacology (Società Italiana di Farmacologia – SIF)
•Francesco Perrone – Clinical Trials Unit, IRCCS National Cancer Institute “Fondazione Pascale”, Napoli
•Carlo Petrini – Bioethics Unit and Ethics Committee, Italian National Institute of Health (Istituto Superiore di Sanità), Roma
•Filippo Pieralli – Internal Medicine and Intermediate Care Unit – General and University Hospital Careggi, Firenze and Italian Scientific Society of Internal Medicine FADOI (Federazione delle Associazioni dei Dirigenti Ospedalieri Internisti)
•Gabriele Puglisi – Department of Biomedical Sciences, Dentistry and Morphological and Functional Imaging, University of Messina
•Giorgio Racagni – Department of Pharmacological and Biomolecular Sciences, University of Milano and Italian Society of Pharmacology (Società Italiana di Farmacologia – SIF)
•Alice Ravizza – Use-Me-D, Torino
•Elisabetta Ravot – Healthware Group, Milano
•Giuseppe Recchia – Fondazione Smith Kline, Verona / daVinci Digital Therapeutics, Milano
•Eugenio Santoro – Laboratory of Medical Informatics, Mario Negri Institute for Pharmacological Research, Milano
•Francesco Scaglione – Department of Oncology and Haemato-Oncology, University of Milan / Department of Laboratory Medicine, Niguarda Hospital, Milan
•Angelo Spognardi – Department of Computer Science, Sapienza University, Roma
•Silvia Stefanelli – Stefanelli & Stefanelli Legal Chambers, Bologna-Milano
•Federico Sternini – Use-Me-D,Torino
•Andrea Tomasini – Italian national Association of People with Rheumatological and Rare Diseases (Associazione Nazionale Persone con Malattie Reumatologiche e Rare – APMARR)
•Gianluca Trifirò – Dipartimento di Diagnostica e Sanità Pubblica, Università di Verona e Società Italiana di Farmacologia (SIF)Department of Diagnostics and Public Health, University of Verona and Italian Society of Pharmacology (Società Italiana di Farmacologia – SIF)
•Dominique van Doorne – European Patients’ Academy/EUPATI Non-Profit Organization
The Authors wish to express their gratitude to Peter Gordon Mead for the linguistic revision of the volume.



